Topic 2 Key concepts and Theoretical framework
Menopause is not a one-dimensional experience. It is biological, emotional, and social, shaped by both personal health and the environments where we live and work. For employers and employees alike, understanding menopause requires more than medical facts; it demands a holistic lens.
The Job Demands–Resources (JD-R) Model
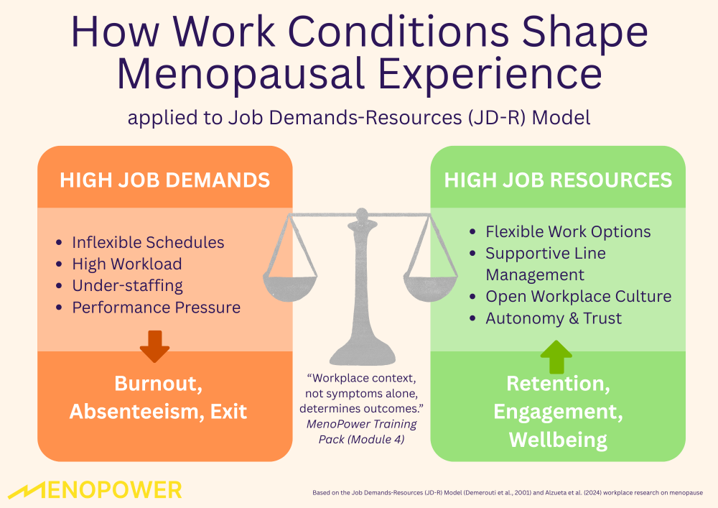
The JD-R Model explains how different aspects of work (both positive and negative) affect employee wellbeing and performance.
Job demands are elements that require sustained physical, emotional, or cognitive effort, such as time pressure, heavy workload, and interpersonal conflict. These demands are linked to stress, burnout, and reduced work ability, especially for employees managing chronic health issues like menopause.
In contrast, job resources, such as autonomy, support from managers, and role clarity, can buffer the impact of high demands, boost motivation, and support retention. The JD-R framework highlights that menopause support must go beyond symptoms and focus on job design and organisational conditions.
The Salutogenic Model of Health
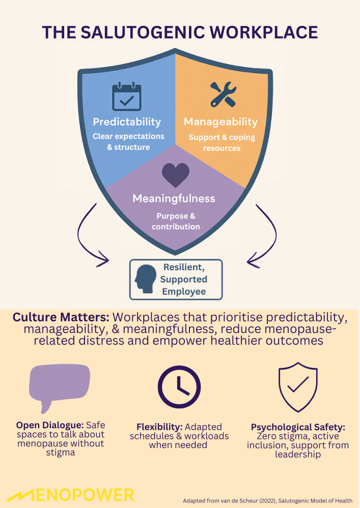
The Salutogenic Model, developed by Antonovsky, shifts the focus from illness to wellbeing. It introduces the concept of a Sense of Coherence, the idea that people stay healthier when their environment is characterised by:
- Comprehensibility (predictability): life feels structured and understandable
- Manageability: people believe they have the resources to cope
- Meaningfulness: they feel their efforts matter and challenges are worth engaging with
Workplaces that foster these elements, through clear expectations, supportive leadership, and emotional safety, help employees stay resilient and healthy during menopause.
Why These Models Matter
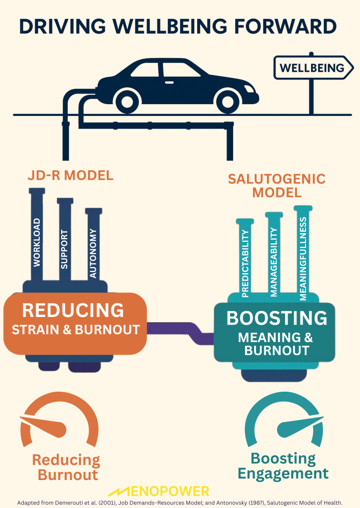
Together, the Job Demands–Resources (JD-R) Model and the Salutogenic Model of Health offer a dual lens for supporting employees through menopause.
- The JD-R Model helps identify and reduce harmful workplace conditions by focusing on the balance between demands and resources.
- The Salutogenic Model shifts attention toward building health-promoting environments, ones that offer clarity, support, and a sense of meaning.
Used together, they help employers move beyond individual adjustments and design systems that protect wellbeing, reduce stigma, and retain talent.
What the Research Shows: Symptoms, Support Gaps & Workplace Risk
Recent studies reveal a widespread gap between what menopausal employees need and what workplaces provide.
- 77.7% of working women experience menopause-related challenges such as fatigue, anxiety, musculoskeletal pain, and brain fog
- Yet only 2–6.3% report receiving any formal workplace support
(Alzueta et al., 2024)
The JD-R model has been applied to this context:
- In high-demand, low-resource environments, menopause symptoms are more likely to lead to burnout, absenteeism, and early workforce exit.
- In low-demand, high-resource environments, employees are more likely to stay engaged, manage symptoms effectively, and remain in the workforce longer.
(Viotti et al., 2021)
These findings confirm that menopause support must go beyond individual awareness and address structural risk factors.
From Insight to Action: What Employers Can Do
Research confirms what many already know: menopause symptoms can affect performance, but only when workplace conditions make it harder to cope.
This isn’t just a health issue; it’s a job design issue.
By aligning with both the JD-R and Salutogenic models, employers can take practical, systemic actions that reduce risk and build resilience.
Over the next slides, we explore five strategies that help turn insight into action, grounded in evidence and adaptable to different workplace contexts.
5 strategies: To turn insight into action
Strategy 1: Adjust Job Roles and Expectations
Menopause symptoms, especially fatigue, anxiety, or brain fog, can make demanding tasks temporarily harder to manage.
Employers can support employees by:
- Reducing workload during symptom flare-ups
- Reassigning non-critical tasks
- Extending or adjusting deadlines
These adjustments protect performance and wellbeing without requiring formal leave. Research shows that temporary flexibility, especially when tied to autonomy, significantly improves outcomes.
Strategy 2: Flexible Working Arrangements
Flexible working helps employees manage fluctuating energy levels and cognitive load during menopause.
Offering options such as:
- hybrid work
- staggered hours, or
- microbreaks
can reduce stress and improve retention.
Research shows that schedule flexibility is linked to higher work ability and greater staff retention for midlife employees.
Even small adjustments in timing and location can make a meaningful difference.
Strategy 3: Managerial Training
Managers play a critical role in shaping whether menopause support succeeds or fails. Targeted training helps them recognise symptoms, respond with empathy, and understand legal responsibilities.
Training should include:
- How to handle disclosures with sensitivity
- When and how to offer adjustments
- Legal frameworks and organisational policies
Evidence shows that supportive leadership significantly reduces burnout and turnover.
Strategy 4: Policy Integration
Menopause support should not rely on individual goodwill, it must be built into policy.
Integrating menopause into workplace health, occupational safety, and DEI frameworks ensures consistent, system-wide support.
Effective policies should clearly outline:
- Available accommodations
- Confidentiality protections
- Anti-discrimination measures
Embedding menopause into broader strategies reduces stigma and protects employee rights.
Strategy 5: Safe Disclosure and Support Channels
Many employees hesitate to speak up about menopause for fear of stigma or career impact.
Employers can reduce this barrier by creating both formal and informal support options, such as:
- Access to HR or trained line managers
- Peer support groups
- Confidential advice lines
These channels promote psychological safety and align with the Salutogenic Model’s emphasis on predictability and emotional support.
Simon Sinek highlights the importance of empathy and creating psychologically safe workplace environments, encouraging leaders and colleagues to foster supportive spaces where employees feel comfortable sharing challenges and seeking help.
EMBEDDED LINK TO VIDEO: https://youtube.com/shorts/YzF3I_uv0Qo?si=YoCGzGPIZJOC5vgT

Legal & Ethical Responsibilities: The EU Context
In the EU, employers are required to protect employee health and prevent discrimination, with potential implications for menopause-related risks.
Key legal frameworks, while not mentioning menopause specifically, set important principles that can be interpreted to support action:
- Directive 89/391/EEC: Requires employers to assess and manage psychosocial and gender-specific workplace risks. While menopause is not named, this duty is broad enough to encompass risks arising from menopause symptoms when relevant to worker wellbeing.
- Directive 2006/54/EC: Prohibits discrimination on the basis of sex, which, according to some interpretations, could include negative treatment linked to menopause.
- ISO 45003 (2021): Offers voluntary guidelines for managing psychological health at work, including gender and health-related considerations, though not legally binding.
- Example: Germany’s Equal Treatment Act (AGG): Requires employers to prevent sex-based discrimination. The underlying principle can reasonably be inferred to apply to menopause, even though it is not named explicitly.
Menopause protection is not explicitly stated in EU workplace law, but existing requirements on health and discrimination can be extended to cover menopause through interpretation and best practice.
Adding menopause-sensitive policies goes beyond baseline compliance, signaling inclusion and modern, evidence-based risk management.
These legal and best-practice frameworks do not make menopause an explicit statutory category, but they strongly support embedding menopause awareness and support within general workplace health, safety, and inclusion strategies. By doing so, employers demonstrate proactive, inclusive, and progressive workplace leadership.

Measuring Impact: How to Track Menopause Support Effectively
To evaluate whether menopause support is working, employers should track both quantitative and qualitative indicators.
Key metrics include:
- Absenteeism and presenteeism rates before and after interventions
- Retention and turnover rates for employees aged 45–55
- Uptake and satisfaction with support resources
- Staff surveys assessing workplace climate and inclusivity
- Participation in training and awareness programs
These metrics help organisations move beyond intention to evidence-based improvement.
Effective menopause support depends on both targeted training and ongoing communication.
Key training priorities:
- Symptom awareness and empathetic response
- Legal responsibilities and policy knowledge
- Signposting to internal and external resources
Best practice suggests:
- Mandatory training for managers and HR
- Accessible content for all employees
- Regular campaigns (newsletters, posters, webinars) to normalise menopause as a workplace issue
These efforts reduce stigma, improve confidence, and ensure menopause is treated as a legitimate part of occupational health
Intersectionality and Inclusivity
Menopause is not experienced the same way by everyone. Factors such as ethnicity, disability, income, and sexual orientation can shape both symptom severity and access to support.
- Some individuals, such as shift workers, LGBTQ+ employees, or non-native speakers, may face additional barriers in workplace policies and care pathways.
- Trans men may experience induced menopause through medical transition, while lesbian individuals may have unique experiences with hormone therapy.
To ensure fair access and effectiveness, menopause strategies must be co-designed with diverse employee voices and tailored to real workplace roles and needs.

Limitations and Future Research
While the JD-R and Salutogenic Models offer robust frameworks for workplace support, current research still leaves important gaps:
- There is limited evidence on how menopause policies perform across different sectors, job types, and cultural settings.
- Experiences of marginalised groups, including ethnic minorities, disabled women, trans men, and non-binary individuals, remain underexplored.
- Longitudinal studies are needed to assess how well workplace interventions improve health, retention, and wellbeing over time.
Building inclusive, evidence-based strategies means acknowledging these gaps, and staying open to future learning and employee-led adaptation.
